As the cases of respiratory illness are increasing day by day UK, US, EU, and many other countries are currently in some degree of "lockdown" hoping that lockdown will halt the spread of COVID-19. Almost 192 countries are being affected by this virus and so at least peoples are asked to stay home, avoid other contacts. Researchers are doing their best on discovering vaccines and treatments for the virus, but it is estimated that even in a best-case scenario, these are likely to be 12-18 months away.
Until a perfect medical solution will not be discovered everyone is suggested to keep enough social distancing and break the chain of transmission. But do lockdown exactly work? To find this a research team Imperial College COVID-19 Response Team studied "Impact of non-pharmaceutical interventions (NPIs) to reduce COVID19 mortality and healthcare demand" and published their result on 16 March 2020.
In the absence of a COVID-19 vaccine, the team assesses the potential role of a number of public health measures – so-called non-pharmaceutical interventions (NPIs) – aimed at reducing contact rates in the population and thereby reducing transmission of the virus. The research was conducted by applying a previously published microsimulation model to two countries: the UK (Great Britain specifically) and the US.
As a result, the team concluded that the effectiveness of any one (mitigation or suppression) intervention in isolation is likely to be limited, requiring multiple interventions to be combined to have a substantial impact on transmission. This report considered the feasibility and implications of both strategies for COVID-19, looking at a range of NPI measures. Also, the report added, "the impact of many of the NPIs detailed here depends critically on how people respond to their introduction, which is highly likely to vary between countries and even communities."
According to the report The goal of the lockdown is to keep reproduction, or "R" below one (R<1) – with each case infecting fewer than one other person, on average. For this, the following two fundamental strategies are possible:
-
Suppression: Under this strategy NPIs and drugs, if available, are to be maintained sporadically for as long as the virus is circulating in the human population, or until a vaccine becomes available. This strategy is challenging as in the case of COVID-19 it is estimated that it will be at least 12-18 months before a vaccine is available and more importantly there is no guarantee that initial vaccines will have high efficacy to cure them.
-
Mitigation: Here the aim is to use NPIs (and vaccines or drugs, if available) not to interrupt transmission completely, but to reduce the health impact of an epidemic. In this scenario, population immunity builds up through the epidemic, leading to an eventual rapid decline in case numbers and transmission dropping it to low levels.
The report provides the result with lockdown a more effective way of stopping the transmission of the COVID-19.
They expected under the scenario without lockdown 81% of the UK and US populations would be infected, with 510,000 dying in the UK and 2.2 million dying in the US.
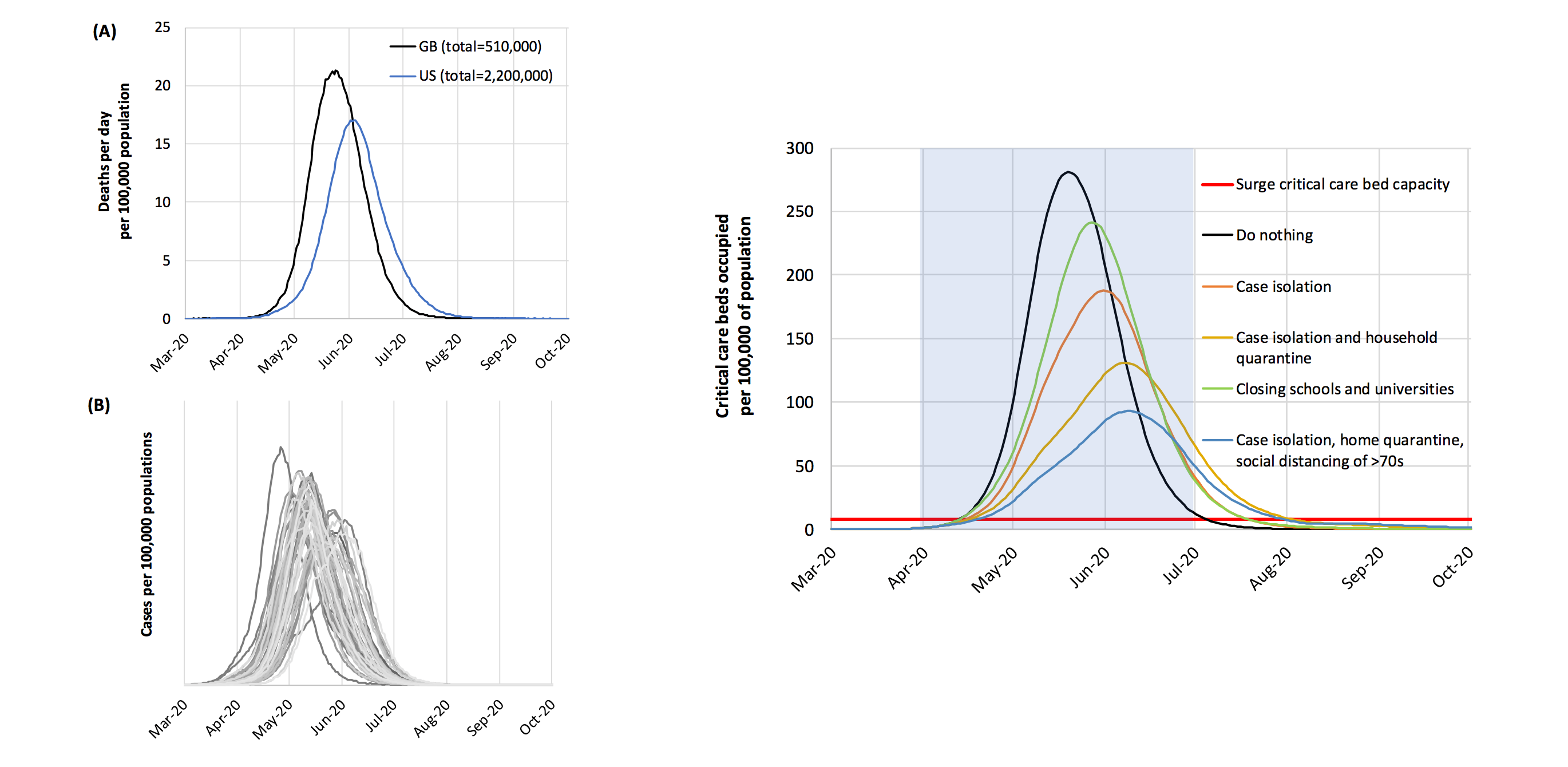
The study reports, "for an uncontrolled epidemic, we predict critical care bed capacity would be exceeded as early as the second week in April, with an eventual peak in ICU or critical care bed demand that is over 30 times greater than the maximum supply in both countries."
The result of the report suggests that to suppress transmission below the threshold of R=1, population-wide social distancing and in combination with home isolation of cases and school and university closure applied to the population as a whole would have the largest impact.
The study also suggests, over time if the case numbers fall suppression might also evolve as a more effective approach.
Analyzing the data from the UK (Great Britain specifically) and the US, the team concluded that epidemic suppression is the only viable strategy at the current time to limit the coronavirus.
References and Further Reading:
-
Impact of non-pharmaceutical interventions (NPIs) to reduce COVID19 mortality and healthcare demand, DOI: 10.25561/77482
